Stepping Right: The Importance of Proper Footwear for Flat Feet
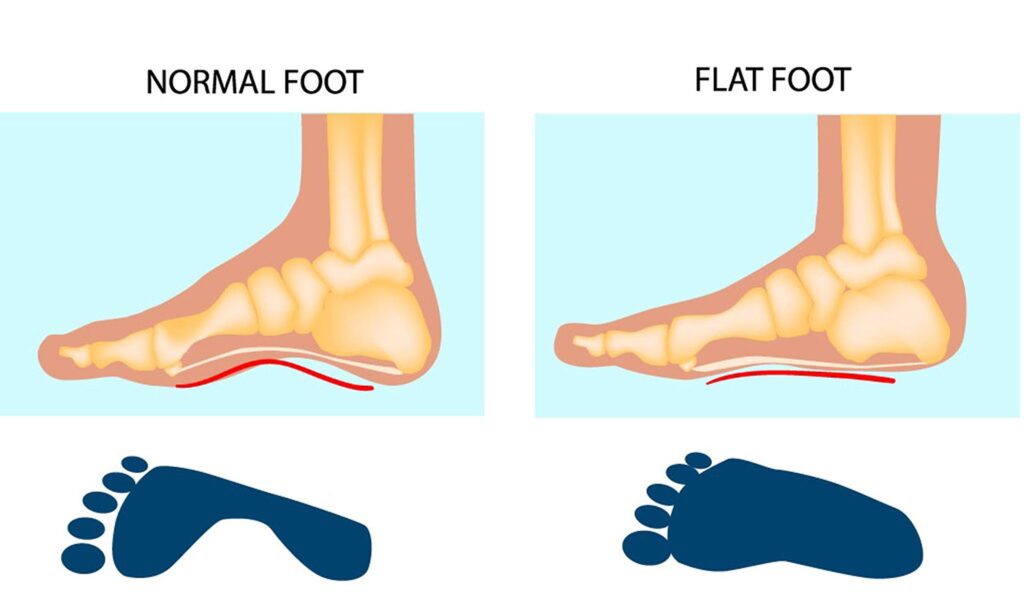
Living with flat feet, or fallen arches, can sometimes feel like walking on uneven ground. Discomfort and even pain can often be managed with the right approach, particularly when it comes to footwear. Choosing supportive shoes specifically designed for flat feet can significantly improve your foot health and overall well-being. Understanding Flat Feet: Flat feet simply occur when the arches of your feet collapse, causing the entire sole to make contact with the ground when standing. This can happen naturally or develop over time due to various factors. The Impact of Improper Footwear: Wearing shoes without proper support can worsen the discomfort associated with flat feet. Lack of support can strain the arches, leading to misalignment and potentially causing pain in the feet, ankles, knees, hips, and even lower back. Choosing the Right Shoes: Arch Support: Prioritize shoes with built-in arch support or consider adding orthotic insoles for additional lift and stability. Stability and Cushioning: Opt for shoes with cushioned soles to absorb shock and provide comfort during movement. Look for features like a firm heel counter to prevent excessive inward rolling (\”overpronation\”) of the feet, a common challenge for those with flat feet. Roomy Toe Box: Choose shoes with a wider toe box to accommodate any natural splaying of your toes. Avoid shoes that crowd your toes, leading to discomfort, especially when your arches flatten under pressure. Flexibility: Opt for shoes with flexible forefoot areas to allow for natural movement while walking or running. Stiff shoes can restrict movement and increase discomfort. Quality Materials: Invest in breathable and durable materials like leather or mesh to promote airflow and prevent moisture buildup, potentially leading to fungal infections and odors. Shoe Recommendations: Athletic Shoes: When engaging in physical activities, choose athletic shoes designed for your specific sport or activity. Many brands offer models with enhanced support and stability features tailored to various exercise needs. Casual and Dress Shoes: For everyday wear, opt for supportive sneakers, loafers, or sandals with arch support and cushioning. Avoid flat shoes like ballet flats or flip-flops, as they offer minimal support and can exacerbate flat feet symptoms. Conclusion: Investing in proper footwear plays a vital role in managing flat feet and promoting overall foot health. By choosing shoes with adequate support, stability, and cushioning, you can alleviate pain, reduce strain on your feet and lower body, and experience greater comfort and mobility in your daily activities. Remember, consulting a podiatrist or healthcare professional can provide personalized advice and recommendations based on your specific needs and foot conditions.
Stepping Right: The Importance of Proper Footwear for Flat Feet Read More »